The Centre for Research on Health Equity and Social Inclusion (CRHESI) is an interdisciplinary, collaborative initiative led by the Faculty of Health Sciences at Western University.
The concepts of health equity and social inclusion cut across the work of many faculties and community service organizations within Western University and the London Not-for-Profit-Sector respectively. CRHESI strives to provide a forum for research-enabled, synergistic and catalytic change for London and surrounding areas.
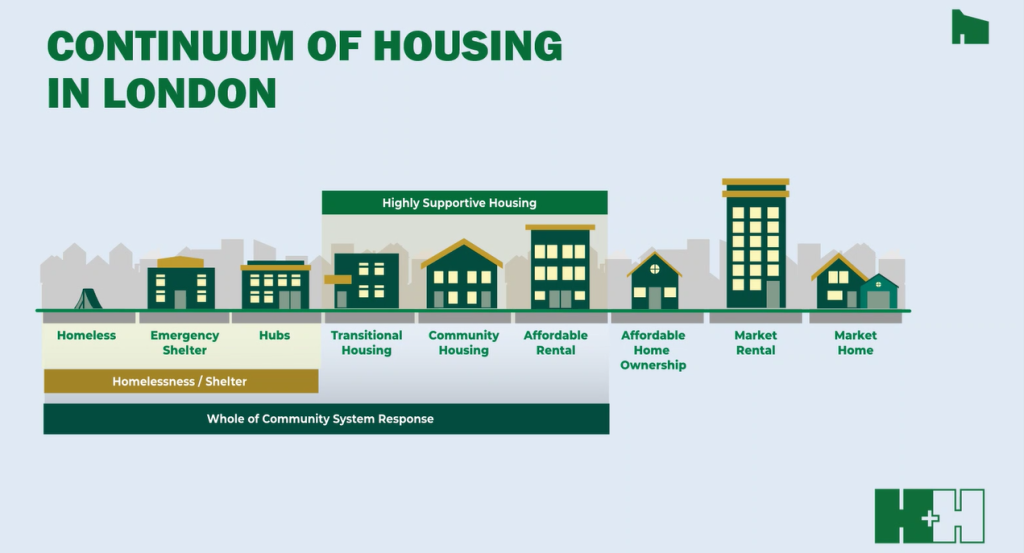
Advocating for Housing
CRHESI UPDATES
-
Webinar: Let’s Talk Moving Upstream – Opportunities for Public Health Action
The National Collaborating Centre for Determinants of Health (NCCDH) is hosting an upcoming webinar exploring opportunities to move public health action further upstream. This foundational learning opportunity will introduce the NCCDH’s updated Let’s Talk: Moving Upstream resource and explore the stream analogy commonly used in public health to understand downstream, midstream, and upstream interventions. Participants…
-
Storyhouse Feature: “My Friend Daniel, Homelessness, and Hope”
CRHESI is pleased to share a new Storyhouse narrative titled “My Friend Daniel, Homelessness, and Hope.” The piece explores homelessness, human connection, and the importance of hope through an accessible storytelling approach grounded in research and lived experience. Storyhouse is a knowledge mobilization initiative connected to Western University that uses creative storytelling to help connect…
-
Invitation: Advancing Action on Anti-Black Racism in Healthcare – May 30, 2026
In June 2025, Western University’s Centre for Research on Health Equity and Social Inclusion (CRHESI) hosted a collaboratively planned event called ‘Addressing Anti-Black Racism in Healthcare’. Information about this event and the input provided by participants can be found here: Addressing Anti-Black Racism in Healthcare: Insights and Calls to Action from London’s African, Caribbean and…
-
Participants Needed for Research on Improving the Wellbeing and Capacity of Frontline Service Workers
Researchers in the Faculty of Health Sciences at Western University are seeking participants for a community-based participatory action research project exploring the use of arts-based and embodied learning methods to support frontline service providers in the social services and community health sectors. The study focuses on collaborative and creative educational approaches to supporting the wellbeing,…
CRHESI PRIORITIES
OUR PARTNERS
CRHESI is grounded in the strong tradition at Western University of conducting research with and for individuals who have experienced vulnerability and marginalization. Our work is made possible through collaboration with a broad network of community and university partners.
Community Organization Partners
- London InterCommunity Health Centre
- United Way
- London Cross Cultural Learner Centre
- Merrymount Family Support & Crisis Centre
- Canadian Mental Health Association (Middlesex)
- My Sister’s Place
- Family Service Thames Valley
- mindyourmind
- Goodwill Industries
- Pillar Nonprofit Network
- London Homeless Coalition
- Muslim Resource Centre
- Southwest Local Health Integration Network (LHIN)
- Middlesex-London Health Unit
- City of London
Western University Partners
- Faculty of Health Sciences
- Faculty of Social Sciences
- Indigenous Health and Well-being Initiative (IHWI)
- Faculty of Information and Media Studies
- Schulich School of Medicine & Dentistry
- Vice Dean, Basic Medical Sciences
- Schulich Interfaculty School of Public Health
- Faculty of Law
- Faculty of Education
- Department of Women’s Studies and Feminist Research
- Brescia University College
- King’s University College – School of Social Work and Poverty Research Centre